If you catch measles, what are your chances of dying?
When I was a kid, measles was one of those things you were expected to catch. I had it when I was five, and must confess, I don’t remember much about the experience. I do remember being confined to bed. And I also remember being told that measles could cause blindness – as a budding reader, this scared me. But I don’t recall anyone hinting at anything worse. If my parents were worried, they didn’t show it. And I’d certainly never heard of kids who had died – even in playground rumors.
So as the current outbreak of measles in the US continues to spread, I’ve been intrigued by statements that the disease has a mortality rate of somewhere between one and three young children per thousand infected.
Of course I know as a public health academic that measles is highly infectious and can cause severe harm – even death. But there was a dissonance between what I was reading and what I felt was correct. Surely if one out of every few hundred kids died as a result of measles as I was growing up, I’d have got wind of it?
The mortality rate of around 1 in 1000 though comes with a sound provenance. It’s there in black and white on the Centers for Disease Control and Prevention (CDC) web pages:
“For every 1,000 children who get measles, one or two will die from it”
A 2004 review in the Journal of Infectious Diseases provides further insight. Using CDC data on reported measles cases in the US between 1989 and 2000,Orenstein, Perry and Halsey indicated that approximately three children under the age of five died for every thousand that caught measles, and that the overall mortality rate for all ages was also around 3 per thousand people infected – the table below gives the data they used in deaths per thousand cases.
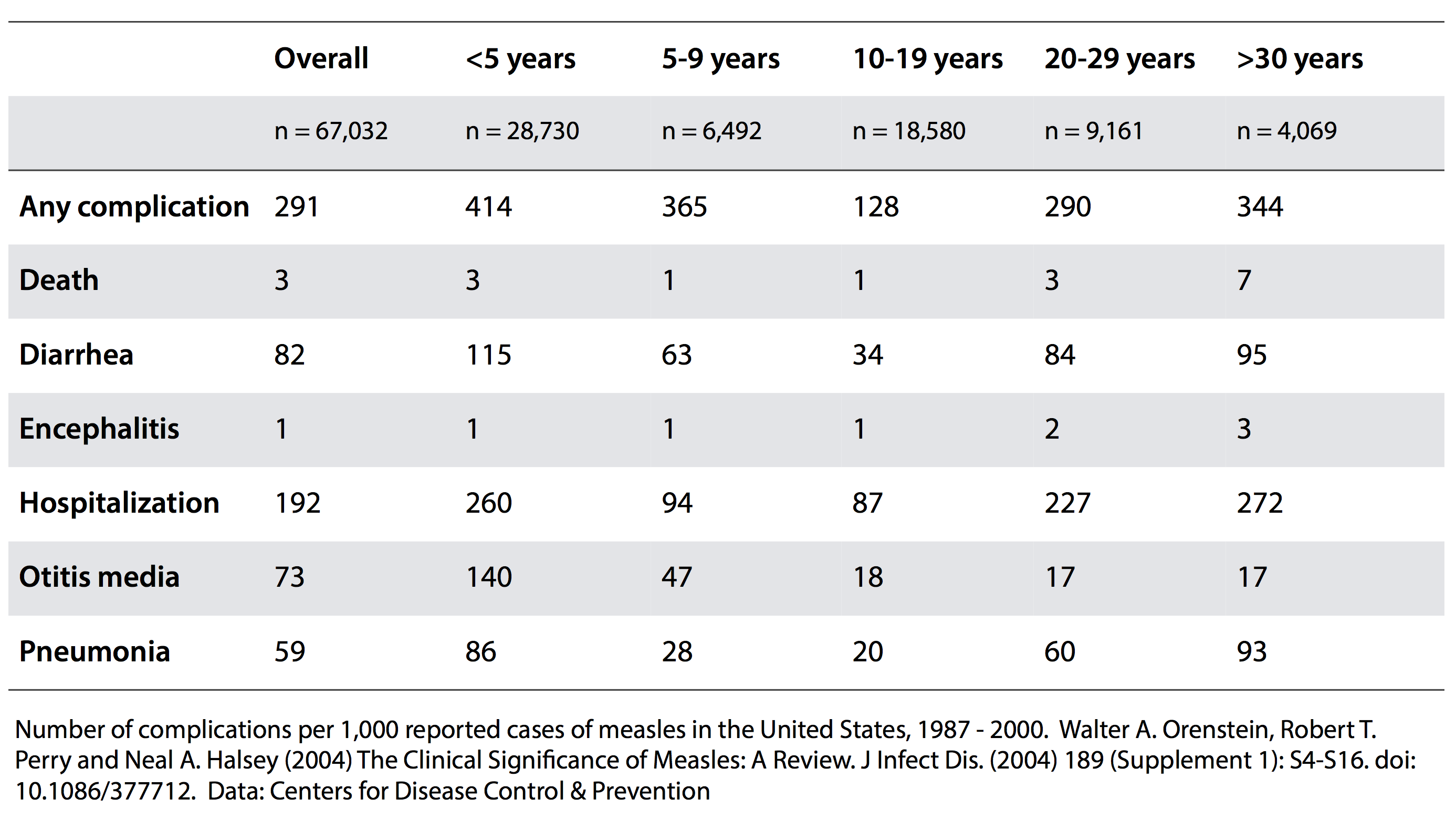
Measles mortality rates in the US 1987 – 2000
This seems pretty convincing – maybe measles is more dangerous than we used to think back in the 70’s.
But there’s a catch.
The CDC dataset that Orenstein, Perry and Halsey used specifically refers to reported cases of measles. The derived mortality rate is for cases that are serious enough to have been flagged and logged by the agency. The question then becomes, how many cases occurred that weren’t reported, and how (if at all) do these alter the estimated mortality rate?
In a 2004 review entitled “Measles Eradication in the United States” (an optimistic title, in the light of current events), Orenstein, Papania and Warton make the point that not every case of measles in the US is reported, or at least it wasn’t, when the disease was more common.
According to their paper, from 1956 to 1960, there were an average of 450 measles-related deaths reported each year in the US, or approximately 1 death per 1000 reported cases. At the time though, it was estimated that more than 90% of Americans had been infected by measles by the age of 15 – equivalent to roughly 4 million children and teens per year. (Langmuir, A.D. (1962), Medical Importance of Measles. Am J Dis Child 103(3):224-226.)
These data suggest that the chances of dying from measles in the US in the late 1950’s was probably closer to 1 in 10,000.
Accounting for non-reported cases that led to death, and some uncertainty in the numbers, the mortality rate is realistically likely to be around one in a few thousand. But based on the data, it’s not likely to be as high the one or two deaths per 1,000 that’s being widely cited.
That shouldn’t detract from how important it is to prevent measles, and especially to protect young children, the elderly and other susceptible groups from infection. This is not a disease to be dismissed or taken lightly. It still kills nearly 150,000 people a year around the world according to the World Health Organization. It is highly infectious. And for communities to be adequately protected, there need to be high levels of immunization.
Yet from the available evidence, claiming that one or two children out of every 1,000 infected in the current US outbreak will die seems far fetched.
Sadly, using this mortality rate to hammer home the importance of getting kids vaccinated could well backfire. Like myself, many parents from my generation haven’t seen evidence for such a high chance of dying from the disease. And to use data that not only feel wrong, but are not backed up with evidence, only serves to undermines trust in public health experts.
Anti-vaccine proponents are smart enough to realize this. Each time the data on infectious diseases and risk are spun beyond their legitimate bounds, anti-vaccine proponents are given a helping hand in winning the hearts and minds of concerned parents.
Instead, public health experts and their advocates need to remain true to the data that support their message. Granted they won’t always be clear and compelling. But this should never be an excuse to spin the data to fit the story.
Ironically, for many people it’s not the numbers that count when it comes to making decisions over whether to vaccinate or not, so much as who to trust. But in deciding whom to place that trust in, numbers – and how they are used – can be very important indeed.
Update Feb 4 2015: A follow-up analysis of data from the 2008-2011 measles outbreak in France has been posted here
Image: Crowd at Disney, by Babs barning, Flickr. Creative Used under Commons License


Interesting, thanks Andrew. I thought somewhat the same thing. I saw the figure 1 in 1000 and thought perhaps it was a different time. But the reported vs the unreported cases makes complete sense. I recall having measles, mumps, and chicken pox all in my tweens. These were uncomfortable but not devastating. Scarlet fever was a different story.
Yeah, when I was checking up on the dates I had measles my mother reminded me that Scarlet Fever was the one people really feared.
And if you look at the Scarlet Fever death and incidence graph, both declined in a similar manner to measles. BUT we can’t say that it was totally without a vaccine, because there was indeed an early scarlet fever vaccine. There are some very interesting medical articles about that scarlet fever vaccine which had such a BAD reputation and ruined the careers of many of the nurses it was trialled in… and while USA tried to persevere with it for years, the response from parents and the medical profession was so violently negative (as opposed to the positive spin the medical system tried to put out there) that they pulled the vaccine and tried never to mention it ever again.
Another piece of medical history which historians appear not to know, or choose not to discuss.
Even today with “modern” more advanced science…, a vaccine for streptococcus pyogenes or group A beta-hemolytic streptococcus, has proved to be elusive.
Very interesting and helpful analysis, Andrew. One angle though that’s problematic for all of us is vulnerability. As you say, the evidence is especially compelling for vulnerable groups – young and elderly. No doubt the risk may exceed one or two in 1,000 for them – trouble is, we can’t know in advance who they are – . Is the cut-off age of special vulnerability 1 year, 3 years..does my child have a yet un-diagnosed condition that makes her more susceptible? So while I appreciate the importance of getting the numbers right, the impact of the fudge factors depends on which side of the split hairs you fall.
Thanks Carolyn. Yes, this is part of the rationale for blanket vaccination and is driven by susceptibility and morbidity as well as mortality. However, if exaggerating risk for the majority of those exposed makes it harder to persuade people to have their kids vaccinated, the result is an increase in risk vulnerability that could otherwise be reduced.
Rational exposition! Go Figure. Thanks for the analysis.
Thank you Andrew. Always important to know both the facts and the context around the facts. Too much of the discussion around vaccines or other risk issues center around some “fact” grabbed out of context. I have read many “fact” based arguments by anti-vaccine parents that clearly lack an appreciation for the basic scientific foundation underlying the so-called “facts.” When I was five, I had the trifecta of measles, chicken pox and rubella (called the three day measles). I certainly remember being sick was no joke. I recently found my kindergarten records and observed that I missed an incredible number of days.
While reassuring Andrew, when we deal with the phenomenon of societal risk/burden sharing, statistics and rational arguments don’t hold much water. One person’s risk taking that may put a larger population at risk is a no-go area, no matter how irrational. If a little boy’s peanut butter sandwich can be taken away because there might be someone in class with an undetected allergy then sending unvaccinated children home makes perfect sense, regardless of the numbers. Couple that with the communal risk/precaution identification, then the families who reject vaccination are ostracized by the crowd (in this case, I believe rightly so, but often the stigmatization is illegitimate). As it has commonly been said, a person may be sensible, but people are stupid (and social media is accentuating this!)
Certainly David the numbers usually aren’t the main factor in personal decisions. But how people use numbers is used as a litmus test for trustworthiness – or as a way of undermining trust. Which is why they matter, even when it seems like they don’t.
We are living in an era where lies are perpetrated in the news and social media. We go to war over false claims of weapons of mass destruction, congress votes bailouts for banks to big to fail, and news anchors are caught in outright lies. And then you have health experts deliberately spinning the facts to try to convince skeptical parents to vaccinate. I know of a couple with twins, a boy and a girl. The children were perfectly normal, but within two weeks of getting vaccinated showed signs of autism. The boy if more affected than the girl, but both are afflicted, and the parents are convinced that it was the vaccine. Next time you wonder why anyone would resist vaccination, maybe you won’t wonder so much.
Thanks Richard. As you probably know, research hasn’t been able to show any causal link between autism and vaccines. Yet as a parent I am all too aware of the desperate desire to find some explanation for when awful things happen to your kids – and we’re biologically preprogrammed to see connections between events in a way that is sometimes extremely hard to resist.
This is in part why trust is so important in overcoming the natural tendency to see connections where there aren’t any, and making decisions as a result that do more harm than good.
I understand your points, but I have a couple of questions:
First off, since measles was less common in the 1990s than the 1950s, wouldn’t a higher percentage of mild cases be reported in the 1990s than in the 1950s? Thus it would seem that, if the rate of underreporting was significantly greater for minor cases than those resulting in death, that the ratio of reported deaths to reported cases should have gone down in the 1990s as compared to the 1950s. However, this doesn’t seem to have happened, given the data you present.
Second, I was under the impression that people who “die from measles” often die from secondary complications, such as pneumonia. Thus it seems like deaths, from complications of the measles, might be reported under different conditions, such as pneumonia or hepatitis. Could this not lead to underreporting of measles related deaths?
Thoughts?
Hi Peter,
Both important points, and ones that highlight the need for more analysis in this area. I don’t have any good answers here, apart from evidence from a number of studies that the mortality rate seems to come out at about 1 – 2 per 10,000 cases. More work needed methinks.
Comment to Peter above.
With H1N1 one of the harshest co-morbidities which contributed to deaths was obesity which causes the immune system to response in a less efficient manner than non-obese.
If you’ve studied the medical literature you will see that the groups at highest risk, were and are people with co-morbidities such as a seizure disorder, Downs syndrome, or a cellular immune system defect such as T-cell disease, or those with chemically coshed immune systems such as cancer or steroidal treatment. Obesity never used to be a serious issue, but not it’s become a public health issue, it may also be a risk factor for measles. That remains to be studied.
Measles deaths are always attributed to measles, not pneumonia; never the underlying co-morbidity….., and the public aren’t usually told about those co-morbidities. But you can usually find the numbers in any medical articles which decide to tell the whole story. The percentage of measles deaths with people with comorbidities depends on the outbreak. In UK when they analysed the risk benefit of measles vaccination looking at who got measles, they acknowledged that 50% of deaths in the 60’s were in people with co-morbidities, but felt that the vaccination programme was worth it. You can find that in the editorial of the August 1st Lancet 1981. In the country I live in, measles deaths are most predominant in people with co-morbidities.
Furthermore recent studies here have found that we have third world rates of vitamin A, D and macro and micronutrients and measles hospitalisations are over-represented in those groups. That is similar to USA, in the medical studies which looked at USA hospitalisations for measles and found that children with measles had vitamin A and other nutrient deficiencies. The efficiency of the cellular immune system is reliant upon the immune system having the right macro and micronutrients, and those factors apply to both complications and deaths. That is why vitamin A given to measles cases in Africa reduced the complications and deaths by 90%.
That’s a story that isn’t being discussed in the hype about 100+ cases of measles in the USA right now. Why are people not being told to look to their vitamin A? Is it presumed that because you have enough to eat, your body has enough to do a job?
So like every true story, there are nuances, and untold issues which can have major impacts on individual and population outcomes.
This is an unusual way to frame the issue, given that we can drive the measles death rate to nearly zero by vaccination. Since there will always be some children who can’t get the vaccine, another way to frame it would be risks to children who cannot be vaccinated. Clearly there are outcomes other than death which we’d be worried about here.